
Dr. Sangeeta Sharma
Senior Gynaecologist & Cosmetic Surgeon
Cosmetic Gynecology
Cosmetic Gynecology, or Female Cosmetic Genital Surgery (fcgs), is the fastest growing subspecialty for women. It includes procedures to enhance the aesthetic appearance of the vulva/vaginal region; and vaginal repairs to enhance or restore sexual function that are degraded due to childbirth or aging. It is practiced by gynecologist, especially urogynecologist, and plastic surgeons.
Cosmetic gynecology is not a medical requirement. It is a trend, driven by women themselves, and not by their sexual partners. Research has shown that the appearance of a woman’s genitalia affects her self-confidence and sexuality.
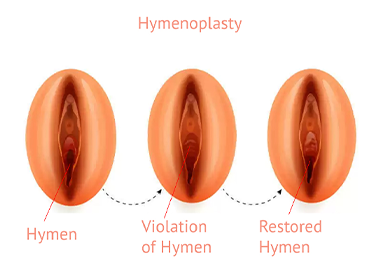
Hymenoplasty
A surgical procedure to reconstruct the hymen for personal, cultural, or psychological reasons.
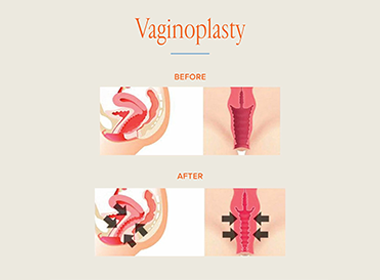
Vaginoplasty
A vaginal tightening procedure that improves tone and strength of vaginal muscles, often after childbirth or aging.
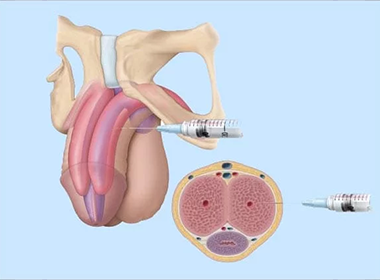
PRP Vaginal Rejuvenation (O-Shot)
Platelet-rich plasma therapy enhances tissue regeneration, improves lubrication, and heightens sexual pleasure.
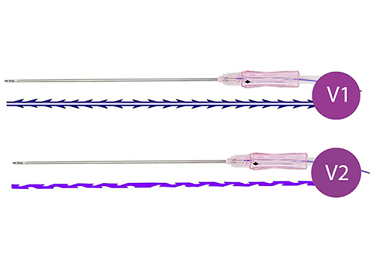
COG Threads for Vaginal Rejuvenation
Absorbable threads are placed to tighten the vaginal wall, stimulate collagen production, and improve tone.
G Shots
A non-surgical option using PRP enhances sexual wellness, sensation, and confidence.
The five main procedures of Cosmetic Gynecology are:
- Hymenoplasty: creating an intact hymen broken by cycling, horse riding or first intercourse. In most countries intact hymen denotes virginity
- Vaginoplasty: tightening of vagina or vaginal rejuvenation, for sexual satisfaction.
- Labiaplasty: improve the appearance of inner labia, and reduce the vaginal lip size.
- Hoodectomy or Clitoral unhooding: remove the tissue that normally covers the clitoris.
- Monsplasty: lift, tighten and shape-up the pubis, the “bikini bridge,” which may be prominent when wearing outfits.
These are minor-surgical, day, procedures. The scar usually is imperceptible; but some amount of bruising, discomfort and swelling is common.
Laser have recently been introduced for vaginal rejuvenation. Lasers have been in wide use for treatments in dermatology and aesthetic medicine. Laser’s introduction to cosmetic gynecology was therefore a natural progression of technology. At present lasers in gynecology are being used for Condyloma, Cervical Dysplasia, Vaginal Tightening, Labial Trimming, Vulvar Melanosis, Liposuction of the Pubis Mound and Vulvar Hair Removal. But the safety and effectiveness of energy-based devices (Laser) for treatment of these conditions has not yet been established.
There is a lack of consensus on technique and outcomes for cosmetic gynec procedures; and potential for damage due to scarring, altered sensation, or wound complications. Coupled with unethical or false claims. Women should be informed about the lack of data supporting the efficacy of these procedures and their potential complications, including infection, altered sensation, dyspareunia, adhesions, and scarring.
Therefore, women opting for cosmetic gynec procedures, beware! Make sure that the gynaecologist you go to is an experienced surgeon.

FAQ's
Laparoscopy is a minimally invasive surgical procedure that uses small incisions and a camera to view and treat endometriosis. It helps identify and remove endometrial tissue outside the uterus, reducing pain and improving fertility.
Laparoscopic surgery for uterine fibroids offers several benefits, including smaller incisions, less pain, quicker recovery, and reduced scarring compared to traditional surgery. It allows for precise removal of fibroids while preserving the uterus.
Yes, laparoscopy is used for both diagnosing and treating endometriosis. During the procedure, the surgeon can visualize the pelvic organs, take tissue samples for biopsy, and excise or ablate endometriotic lesions.
Recovery time after laparoscopic surgery for endometriosis varies, but most patients can expect a few days to a few weeks for a full recovery, depending on the extent of the surgery and individual factors.
Relief from uterine fibroid symptoms can be experienced shortly after laparoscopic surgery, but the exact timeline may vary. Some women report immediate symptom improvement, while others may take a few weeks to notice a significant difference.
Managing endometriosis post-laparoscopy may involve dietary and lifestyle changes. A balanced diet, regular exercise, stress reduction, and hormone therapy, if prescribed, can help alleviate symptoms and promote overall well-being.
Laparoscopy aims to remove uterine fibroids, but complete removal depends on factors such as the size, number, and location of the fibroids. The surgeon will strive to eliminate as many fibroids as possible to reduce symptoms and preserve fertility.
Before undergoing laparoscopic surgery for endometriosis, specific preparations may be necessary. These can include fasting for a certain period, adjusting medications, and undergoing pre-operative tests as advised by the healthcare provider.
Some pain or discomfort is expected after laparoscopic surgery for uterine fibroids. Pain medications, rest, and following post-operative instructions can help manage pain effectively during the recovery period.
The duration of a laparoscopic procedure for endometriosis treatment typically ranges from 30 minutes to a few hours, depending on the complexity of the case, the extent of the disease, and the required interventions. The surgeon will provide a more accurate estimate based on individual circumstances.
